|
Ethics is at the very heart of counselling - every intervention I make when I am sat with someone, is an ethical decision. Being a member of a professional organisation, underpins my ability to be ethical in my practice.
My professional body, the British Association for Counselling and Psychotherapy (BACP), has recently updated its ethical framework, and part of practicing ethically also means engaging with this new document. One way to engage is to go through the document and compare the new requirements with my current practice, and see if I need to make any changes. This is a rather dry thing to do, and something I am not particularly interested in writing about. I am much more interested in looking at how the framework uses language, and how this illuminates the relationship with my professional body. To sharpen the exploration I will be comparing it to the GMC's Good Medical Practice, a similar framework for doctors. What's new?
Comparing new with old, they both have the same layout.
The 1st section is entitled "Ethics" and contains subsections on Values, Principles, and Moral Qualities. The most notable change in the new framework is that this section is shorter - the Principles which form the core of ethical decision making, no longer have a definition. The biggest changes are in the 2nd section, which in the old version was called "Guidance on Good Practice". In the newer version the word "Guidance" no longer appears, and is simply called "Good Practice" There is a good reason for that. In the original framework this section did read very much like guidance, whereas in the new you are presented with a set of standards. Is the BACP's framework, still a framework?
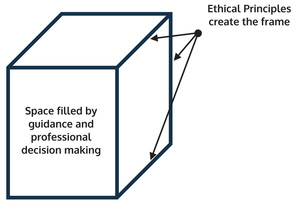
The old framework was very much like a wire-frame cube, with the ethical principles forming the wires, while the space in between was filled with guidance and professional decision making,
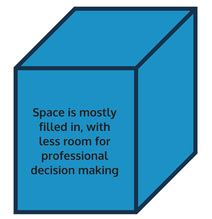
Whereas the new framework is more like this, The new framework marks a significant shift away from guidance, which left many decisions up to the individual practitioner, to one where they are no longer decisions, they are imperatives stated as "we will." One such shift is "accurate record keeping" is now mandatory, where as previously it was advisory. This shift while it has made the framework more clear cut, compared to the sometimes vague and at times wordy older version, has also eroded professional autonomy. I also find the title, "Ethical Framework" rather at odds with the actual contents of the document. The framework has been shrunk, and is less significant, while the good practice section now reads as a code of conduct. It's form is very similar to the GMC version. A more accurate title might be "Ethical Standards in the Counselling Professions" Are the BACP's standards ethical?
This may sound like a strange question to ask, however I have found the BACP's assumption,
Ethical decisions that are strongly supported by one or more of these principles without any contradiction with the others may be regarded as well-founded. to be at odds with my own understanding of working ethically. Ethical decisions always involve contradiction and dilemmas. For Kant the BACP's proposition would have little moral value. Why? Which has more moral worth? Is it the person who when they see someone collapsed in the street goes over to help, with little thought about anything else, because they are inclined to do so? Or is it the person who is uncertain whether to go over, as they also weigh up the harm that could be done to them, and the harm they could cause by trying to help? A Kantian perspective argues that it is the second one. We are at our most ethical when we are struggling with uncertainty of what "doing the right thing" is. This dilemma is central to all helping relationships, and particularly so in counselling. My experience tells me, if a decision involves "no contradiction" then you haven't considered it enough! This is often what supervision is like. I begin with what appears to be a simple decision, which after about 10-15 minutes turns into a dilemma. Acknowledging and working with dilemma is at the heart of ethical practice, and is why supervision is essential to working ethically. The BACP have significantly downplayed uncertainty in ethical decision making, which is reflected in the way the principles are commented upon. The "will inevitably" in the older version has been downgraded to a, "may encounter circumstances in which it is impossible to reconcile all the applicable principles," in the new one. The overall prescriptive nature of the BACP's standards not only implies that doing the right thing is fixed regardless of context, it also implies it is certain and knowable. And while this could be seen to have little ethical value, more importantly it does not fit well with my own experience of counselling. Is the BACP medicalising counselling?
A criticism leveled at the BACP is the influence of medical ethics on the counselling profession, such as this in depth piece by Peter Jenkins.
So is this visible in the final document?
The older framework simply read, "Alleviating personal distress and suffering," symptoms weren't mentioned. From a personal perspective I don't want to alleviate symptoms, I would much prefer to alleviate actual distress and suffering. Also using "symptoms" is not compatible with a humanistic approach. The nearest equivalent concept is something I would call experiential phenomena, which is a fancy way of saying that what we experience are understood to be events. A symptom is a sign of an underlying event. In this case some kind of pathology, which simply means suffering. Where as, an experiential phenomenon is an event all of itself, there is nothing underlying it - it's not a sign of something else. When we refer to symptoms, we are in essence adopting a mechanical view of the body. This is where we assume the body is like a complex machine with a normal range of function. When that machine breaks down, it throws up symptoms, which we can then diagnose and treat, to return the machine back to normal, just as a car mechanic might listen to the sound of your engine, and decide that it needs new spark plugs. This view of humanity is alien to the humanistic tradition, which believes we are all inherently OK, neither good nor bad, we are changing all the time, and form a whole with our environment. While the BACP may be seeking to better align counselling with the medical field, and the growth of things like IAPT, adding the word "symptoms" to values is an unnecessary addition. Leaving it out still allows room for both a medical model and a humanistic model of suffering and distress. There is a further oddity in the section on Principles. They are no longer defined, which for a document which seems to be about increasing certainty, feels counter-productive. This step would be OK, if there was little ambiguity. This is not the case for this Principle, Beneficence: a commitment to promoting the client’s wellbeing. The problem here is that there is no commonly agreed definition of wellbeing. The previous framework defined it as "promoting the best interests of the client," which clearly places the definition within a legal framework, such as the Mental Capacity Act 2005. One definition you might consider, is wellbeing as the absence of ill-health, which would fit with using "symptoms of" from earlier. In a discussion paper,The challenge of defining wellbeing, Rachel Dodge and her team argue that such a definition is inadequate, and go on to propose their own. To me this seems like a strange limbo to leave ethical decision making with. Is the BACP disguising a power imbalance?
The "Good Practice" section is essentially a list of rules about how counsellors should behave. All rules by their very nature contain,
An imbalance of power. For a rule to have any force one group must have power over another. So adults frequently make rules about children, but children are rarely able to make rules about adults. In the GMC's good practice guide this power imbalance is clearly visible, and you will read things like, 14. You must recognise and work within the limits of your competence. Reading the document it is as though the GMC are telling you what you must do to comply with their rules. And of course, the GMC are in a position to do that because you must be licenced by them in order to practice as a doctor. The BACP take a different tact, rather than use "you must," they instead use, 12. We will do everything we can to develop and protect our clients’ trust. So who is deciding the rules here? Apparently 'we' are. So who is this 'we'? Is it the BACP committee? Or is it the BACP members? Or is it perhaps all counsellors in general? What happens if you replace 'we' with 'you' as the GMC does? The document takes on a much more coercive and authoritarian tone, as each statement becomes a 'you will'. In reality the meaning of the document has not changed – it is still a list that I must comply with in order to be a member of the BACP. What has happened is an imposition of will. 'Will' has more than one meaning - more ambiguity. It can be understood to mean 'inevitable', so it would actually be more of an imposition than 'must'. It also has a meaning very much like 'wish' as in 'last will and testament', which is less 'inevitable', and is more like a promise. So by using 'we will' the BACP's will has become my will. Is this really true? Not for all the statements, it's not. I have a particular problem with the absolutist nature of several of the statements, such as 'everything' in no. 12 above. Technically, everything is an infinity – it's a never ending list. Try thinking everything you can about cooking or cars. This doesn't seem particularly reasonable, nor possible. A more realistic statement might say something like, “I will take all reasonable steps to develop and protect my clients' trust.” Here reasonable has an agreed definition – it's what a competent practitioner would do. So what happens if 'we' find the rules unsuitable and want to change them? And this last question is key. My only real power, and I can only talk about me, because I don't know who 'we' are, is to leave the BACP and join another professional body. And it is from within this context that you can understand the use of 'we' rather than 'I' or 'you'. Here 'we' helps to increase acceptance - If I believe others accept the rules, then I am more likely to as well. The BACP are trading on the ambiguity of 'we' - when I read the word, 'we', I have to imagine a group that I am part of, which evokes an emotional reaction - feelings such as belonging, pride, esteem, and so on. This is similar to how politicians use metaphorical language in their speech to persuade us. What happens when wills collide?
I think the most serious flaw in the new standards is that it does not allow for conflicting duties. Whenever 'will' is used then I am “fully and unconditionally committed to fulfilling a specific requirement”
And notice it is fulfilling the requirement I am unconditionally committed to. It follows, I can only fulfill all the requirements as long as there is no conflict between my obligations. I don't have to spend much time examining the document to see that there are conflicting duties. In particular this one is problematic, 11. We will take action to prevent harm caused by practitioners to any client. So imagine if my client comes in and begins talking about someone they know who is seeing another therapist, and then they describe some harm that has occurred. No. 11 says that I am fully and unconditionally committed to take action, however no. 12 says I will do everything I can to protect my clients trust, and no. 7 says I will make each client the primary focus of my work. So, do I ignore no 7. and interrogate my client to find out the name of the therapist so I can take action? What if my client refuses consent for me to take action? Now I am really in a pickle. I can't fulfill no 11. without breaking no 12. To complicate matters even further, if the harm is not sufficiently serious to break confidentiality I do not have a legal leg to stand on either. There are also potential conflicts between, no. 24 “We will challenge colleagues or others involved in delivering related services...” and no. 18 “We will maintain our own physical and psychological health at a level that enables us to work effectively with our clients.” In reality employees in organisations need to have supportive structures that allow for challenge. Putting the onus on individual practitioners, without also putting an onus on the organisations in which they work is unreasonable. With the mixing of wellbeing teams in places like universities, and schools there is potential for significant conflict if one section is seen to be critical of another section, particularly if the other section is bound by a different ethical code. Challenging poor or discriminatory practice may also be problematic when the person you wish to challenge is in a position of authority. In summary
While I may not agree with the language used, I agree with the intention behind the good practice standards. There are areas where I don't agree with the degree of emphasis that has been placed on some of them, some of which I have discussed above.
The things I would like to see the BACP address are,
main picture by Pete Linforth
ReferencesAre you a counselling student looking for personal therapy?
I am an experienced counsellor in private practice in the Southampton area of England, UK. I specialise in offering personal therapy to counselling students as part of their course requirement.
3 Comments
15/2/2017 02:00:51 pm
I am a course leader and lecturer at an FE college, and a student has made reference to this piece.
Reply
Mark Redwood
15/2/2017 05:06:22 pm
Dear Carolyn,
Reply
5/9/2020 03:34:16 am
I agree with the comments about the new ethical framework, with the emphasis on rules as opposed to guidelines.
Reply
Leave a Reply. |
Categories
All
Archives
January 2021
|
BioI'm Mark, a Humanistic Counsellor. |
Home - Testimonials - Articles - Links - Contact - Book Appointment - Counselling Students - Privacy Policy - Terms
Mark Redwood, BA (Hons) Counselling, MBACP
© Mark Redwood 2015, 2016.2017 | Main portrait by Doug Freegard © 2015


 RSS Feed
RSS Feed